Skip to main navigation
Skip to main content
Skip to footer
For
Medicare
For
Providers
For
Brokers
For
Employers
Español
For Individuals & Families:
For Individuals & Families
Medical
Dental
Other Supplemental
Explore coverage through work
How to Buy Health Insurance
Types of Dental Insurance
Open Enrollment vs. Special Enrollment
See all topics
Shop for international insurance plans
Member Guide
Find a Doctor
Log in to myCigna
Home
Knowledge Center
Wellness Library
Biventricular Pacemaker
Biventricular Pacemaker
Treatment Overview
Cardiac resynchronization therapy (CRT) uses a special type of pacemaker called a biventricular pacemaker (say "by-ven-TRICK-yuh-ler") to treat heart failure. This pacemaker sends electrical pulses to make the ventricles pump at the same time.
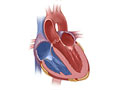
A biventricular pacemaker is implanted in the chest, and it connects to three thin wires, called leads. The leads go into different chambers of your heart. If there is a problem with your heartbeat, the pacemaker sends a painless signal through the leads to fix the problem. The pacemaker also can speed up your heart if it is beating too slowly.
In some cases, you may get a pacemaker that is combined with a device to shock your heartbeat back to a normal rhythm if it is dangerously fast. The device is called an implantable cardioverter-defibrillator, or ICD. It can prevent sudden death.
Your doctor will put the pacemaker in your chest during minor surgery. You won't have open-chest surgery.
Your doctor makes a small cut (incision) in your chest. The doctor puts the leads in a vein and threads them to the heart. Then the leads are connected to the pacemaker. Your doctor puts the pacemaker in your chest and closes the incision. Your doctor also programs the pacemaker.
What To Expect
What To Expect
Most people spend the night in the hospital. This is just to make sure that the device is working and that there are no problems from the surgery. But sometimes the procedure is done as an outpatient procedure, which means you don't need to stay overnight in the hospital.
You might see a little bump under the skin where the pacemaker is placed.
Daily precautions
You'll need to be cautious around certain electric devices. Some devices have a strong electromagnetic field. This field can keep your pacemaker from working right for a short time. These devices include things in your home, garage, and workplace. Check with your doctor about what you need to avoid and what you need to keep a short distance away from your pacemaker. Many household and office electronics don't affect your pacemaker.
Why It Is Done
Why It Is Done
When you have heart failure, the lower chambers of your heart (the ventricles) aren't able to pump as much blood as your body needs. Sometimes the heart has a problem with the electrical system that controls the pumping. This means the ventricles don't pump at the right time or the heart has an abnormal rhythm. A pacemaker for heart failure can help the heart pump blood better.
Whether a pacemaker for heart failure is right for you depends on many medical facts. Your doctor will check many things including: footnote 1
- How bad your symptoms are and if you have trouble doing everyday activities. Heart failure is grouped—or classified—according to symptoms. Your doctor will probably talk about your heart failure "class" number, which will be between I and IV.
- Your ejection fraction. This is a measure of how much blood your left ventricle pumps.
- Your heart's electrical system. You will likely have tests to check for heart rhythm problems.
How Well It Works
How Well It Works
A pacemaker can help your heart pump blood better. It may help you feel better so you can be more active. It also may help keep you out of the hospital and help you live longer.
A pacemaker can slow the progression of heart failure. It can do this by helping the heart's electrical system work well and by changing the shape of your heart. In heart failure, the left ventricle often gets too big as it tries to make up for not pumping well. The pacemaker can slow down this change in your ventricle. It might even help your ventricle go back to a more normal size.
- A large study found that 19 out of 100 people who were treated with a pacemaker for heart failure had to go into the hospital during the study because of heart failure. But 27 out of 100 people treated with medicine alone had to go into the hospital for heart failure.footnote 2
- In the same study, 13 out of 100 people who got a pacemaker for heart failure died during the study, compared with 16 out of 100 who got only medicine.footnote 2
- The combination of a pacemaker and an ICD (implantable cardioverter-defibrillator) can also help people live longer and stay out of the hospital.footnote 3
Risks
Risks
There are several risks to getting a pacemaker. But risks vary for each person. Your doctor can help you understand your risks.
Afterward, you will see your doctor regularly to check your pacemaker and make sure you don't have any problems.
During and soon after the procedure
Problems can happen during or soon after the procedure to implant a pacemaker. Examples of problems include the following:
- Pain, bleeding, or bruising may happen soon after the procedure.
- A lung could collapse (pneumothorax). This happens if air builds up in the space between the lung and the chest wall. This might happen about 1 time out of 100. So about 99 times out of 100, no problems happen.footnote 4
- The doctor might not be able to implant the pacemaker. This might happen if a vein near the left ventricle is too small, too wide, or too hard to reach to allow a lead to be placed. Sometimes the chest or heart may be too big to place a lead.
- Problems during and after the procedure. These might happen about 4 times out of 100. That means problems don't happen about 96 times out of 100.footnote 5
After the procedure
Problems can also happen months or years after the pacemaker is implanted. These problems are related to the device or the leads. Most people don't have long-term issues with their pacemakers.
Problems include:
- Infection in your chest near the pacemaker. An infection might happen about 1 time out of 100. This means that about 99 times out of 100 there is no infection.footnote 6
- The pacemaker or leads might not work. Within a year of pacemaker placement, these problems might happen about 5 to 7 times out of 100. So 93 to 95 times out of 100, the problems don't happen and the pacemaker and leads do work.footnote 5
References
References
Citations
- Heidenreich PA, et al. (2022). 2022 AHA/ACC/HFSA guideline for the management of heart failure: A report of the American College of Cardiology/American Heart Association. Journal of the American College of Cardiology, published online April 1, 2022. DOI: 10.1016/j.jacc.2021.12.012. Accessed April 1, 2022.
- McAlister FA, et al. (2007). Cardiac resynchronization therapy for patients with left ventricular systolic dysfunction: A systematic review. JAMA, 297(22): 2502–2514.
- Tang ASL, et al. (2010). Cardiac-resynchronization therapy for mild-to-moderate heart failure. New England Journal of Medicine, 363(25): 2385–2395.
- Van Rees JB, et al. (2011). Implantation-related complications of implantable cardioverter-defibrillators and cardiac resynchronization therapy devices. Journal of the American College of Cardiology, 58(10): 995–1000.
- McAlister FA, et al. (2007). Cardiac resynchronization therapy for patients with left ventricular systolic dysfunction: A systematic review. JAMA, 297(22): 2502–2514.
- Glikson M, et al. (2021). 2021 ESC guidelines on cardiac pacing and cardiac resynchronization therapy. European Heart Journal, 35(14): 3427–3520. DOI: 10.1093/eurheartj/ehab364. Accessed April 14, 2022.
Current as of: October 2, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Ignite Healthwise, LLC, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.
To learn more about Ignite Healthwise, LLC, visit webmdignite.com.
© 2024-2025 Ignite Healthwise, LLC.
<cipublic-spinner variant="large"><span>Loading…</span></cipublic-spinner>