Treatment Option Overview
There are different types of treatment for children with central nervous system (CNS) atypical teratoid/rhabdoid tumor (AT/RT).
There are different types of treatment for children with AT/RT. You and your child's care team will work together to decide treatment. Many factors will be considered, such as where the cancer is located and your child's age and overall health.
Your child's treatment plan will include information about the tumor, the goals of treatment, treatment options, and the possible side effects. It will be helpful to talk with your child's care team before treatment begins about what to expect. For help every step of the way, see our booklet, Children with Cancer: A Guide for Parents.
Children with AT/RT should have their treatment planned by a team of health care providers who are experts in treating cancer in children.
A pediatric oncologist, a doctor who specializes in treating children with cancer, oversees treatment of AT/RT. The pediatric oncologist works with other health care providers who are experts in treating children with CNS cancer and also specialize in other areas of medicine. Other specialists may include:
- pediatrician
- pediatric neurosurgeon
- radiation oncologist
- neurologist
- pediatric nurse specialist
- rehabilitation specialist
- psychologist
- social worker
- geneticist or genetic counselor
- fertility specialist
Childhood brain tumors may cause symptoms that begin before the cancer is diagnosed and continue for months or years.
Symptoms caused by the tumor may begin before diagnosis. These signs or symptoms may continue for months or years. It is important to talk with your child's doctors about symptoms caused by the tumor that may continue after treatment.
The following types of treatment may be used:
Surgery
Surgery is used to treat CNS AT/RT. Learn more about how this tumor is diagnosed.
After the doctor removes all the cancer that can be seen at the time of the surgery, most children will receive chemotherapy and possibly radiation therapy to try to kill any cancer cells that are left. Treatment given after surgery to lower the risk that the cancer will come back is called adjuvant therapy.
Chemotherapy
Chemotherapy uses drugs to stop the growth of cancer cells. Chemotherapy either kills the cells or stops them from dividing. Chemotherapy may be given with other types of treatments.
Chemotherapy for AT/RT is injected into a vein. When given this way, the drugs enter the bloodstream and can reach tumor cells throughout the body. High doses of some chemotherapy drugs given into a vein can cross the blood-brain barrier and reach the tumor. Chemotherapy for AT/RT is also placed directly into the cerebrospinal fluid (intrathecal chemotherapy). Combination chemotherapy uses more than one anticancer drug.
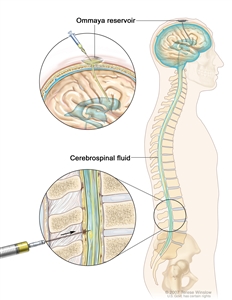
Intrathecal chemotherapy. Anticancer drugs are injected into the intrathecal space, which is the space that holds the cerebrospinal fluid (CSF, shown in blue). There are two different ways to do this. One way, shown in the top part of the figure, is to inject the drugs into an Ommaya reservoir (a dome-shaped container that is placed under the scalp during surgery; it holds the drugs as they flow through a small tube into the brain). The other way, shown in the bottom part of the figure, is to inject the drugs directly into the CSF in the lower part of the spinal column, after a small area on the lower back is numbed.
Chemotherapy drugs used alone or in combination to treat AT/RT in children include:
- carboplatin
- cisplatin
- cyclophosphamide
- cytarabine
- etoposide
- methotrexate
- thiotepa
Other chemotherapy drugs not listed here may also be used.
Learn more about how chemotherapy works, how it is given, and common side effects at Chemotherapy to Treat Cancer.
Radiation therapy
Radiation therapy uses high-energy x-rays or other types of radiation to kill cancer cells or keep them from growing. External radiation therapy uses a machine outside the body to send radiation toward the area of the body with cancer.
Because radiation therapy can affect growth and brain development in young children, especially children who are 3 years old or younger, the dose of radiation therapy may be lower than in older children.
Learn more about External Beam Radiation Therapy for Cancer and Radiation Therapy Side Effects.
Stem cell transplant
High doses of chemotherapy are given to kill cancer cells. This treatment destroys healthy cells, including blood -forming cells. Stem cell transplant is a treatment to replace the blood-forming cells. Stem cells (immature blood cells) are removed from the blood or bone marrow of the patient and are frozen and stored. After the patient completes chemotherapy, the stored stem cells are thawed and given back to the patient through an infusion. These reinfused stem cells grow into (and restore) the body's blood cells.
Clinical trials
For some children, joining a clinical trial may be an option. There are different types of clinical trials for childhood cancer. For example, a treatment trial tests new treatments or new ways of using current treatments. Supportive care and palliative care trials look at ways to improve quality of life, especially for those who have side effects from cancer and its treatment.
You can find clinical trials for people with atypical teratoid/rhabdoid tumor at Treatment Clinical Trials for Atypical Teratoid/Rhabdoid Tumor or use the clinical trial search to find NCI-supported cancer clinical trials accepting participants. The search allows you to filter trials based on the type of cancer, your child's age, and where the trials are being done. Clinical trials supported by other organizations can be found on the ClinicalTrials.gov website.
Learn more about clinical trials, including how to find and join one, at Clinical Trials Information for Patients and Caregivers.
Treatment for childhood CNS AT/RT may cause side effects.
Cancer treatments can cause side effects. Which side effects your child might have depends on the type of treatment they receive, the dose, and how their body reacts. Talk with your child's treatment team about which side effects to look for and ways to manage them.
To learn more about side effects that begin during treatment for cancer, visit Side Effects.
Problems from cancer treatment that begin 6 months or later after treatment and continue for months or years are called late effects. Late effects of cancer treatment may include:
- physical problems
- changes in mood, feelings, thinking, learning, or memory
- second cancers (new types of cancer)
Some late effects may be treated or controlled. It is important to talk with your child's doctors about the effects cancer treatment can have on your child. Learn more about Late Effects of Treatment for Childhood Cancer.
Follow-up care may be needed.
As your child goes through treatment, they will have follow-up tests or check-ups. Some of the tests that were done to diagnose the cancer may be repeated. Some tests will be repeated to see how well the treatment is working. Decisions about whether to continue, change, or stop treatment may be based on the results of these tests.
Some of the tests will continue to be done from time to time after treatment has ended. The results of these tests can show if your child's condition has changed or if the cancer has recurred (come back).
Resources and support are available to help you cope with your child's cancer.
When your child has cancer, every member of the family needs support. Taking care of yourself during this difficult time is important. Reach out to your child's treatment team and to people in your family and community for support. To learn more, see Support for Families: Childhood Cancer and the booklet Children with Cancer: A Guide for Parents.