Skip to main navigation
Skip to main content
Skip to footer
For
Medicare
For
Providers
For
Brokers
For
Employers
Español
For Individuals & Families:
For Individuals & Families
Medical
Dental
Other Supplemental
Explore coverage through work
How to Buy Health Insurance
Types of Dental Insurance
Open Enrollment vs. Special Enrollment
See all topics
Shop for international insurance plans
Member Guide
Find a Doctor
Log in to myCigna
Home
Knowledge Center
Wellness Library
Heart Transplant
Heart Transplant
Surgery Overview
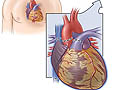
A heart transplant is a procedure in which a surgeon removes a diseased heart and replaces it with a donor heart. During a heart transplant, a mechanical pump circulates blood through the body while the surgeon removes the diseased heart and replaces it with a healthy heart from a recently deceased donor.
The surgeon connects the donor heart to the major blood vessels and hooks the heart up to wires that temporarily control the heartbeat. The procedure takes several hours.
To prevent the body from rejecting the donor heart, your surgeon will give you powerful drugs (immunosuppressants) right after surgery. You must continue to take them.
What To Expect
What To Expect
After a heart transplant, the recovery process is similar to the process after other heart surgeries.
You will spend about 1 to 2 weeks in the hospital after surgery. You may have to stay longer. How long you'll stay depends on your health and if you have complications from surgery. While in the hospital, you will start a cardiac rehabilitation program. And your doctors will check on your heart to make sure your body isn't rejecting it.
Cardiac rehabilitation
A cardiac rehab program can help you recover from your surgery and be active again.
Your transplanted heart will respond to activity a little differently. Your heart rate will not increase like it used to. And you will have a higher resting heart rate. This is because some of the nerves that control your heart were cut during your surgery.
After a heart transplant, you must follow a strict lifestyle involving daily medicines and regular medical care. This includes regular sampling (biopsies) of the transplanted heart tissue to check for rejection.
Learn more
Why It Is Done
Why It Is Done
A heart transplant is an option when the heart no longer works well enough and a person is at risk of dying. A heart transplant may be considered when a person has severe heart disease and is likely to benefit most from a donor heart. A person might be a candidate for a transplant when any of these conditions are true:
- The person has end-stage heart failure, ischemic heart disease, cardiomyopathy, or congenital heart disease.
- The person has a low chance of living as long as 1 year without a heart transplant.
- The person has no other serious medical conditions that would reduce life expectancy.
- The doctor strongly expects that a heart transplant will increase survival and improve the person's quality of life.
At some centers, transplant candidates must demonstrate that they have quit smoking and/or overusing alcohol for a period of time (such as 4 to 6 months) before they are considered for placement on a transplant waiting list.
How Well It Works
How Well It Works
In carefully selected people, a heart transplant can be very successful. About 87 out of 100 people who have a heart transplant survive for at least 1 year. About 60 out of 100 survive 10 years.footnote 1
Most people can have a good quality of life after their transplant. They can be active, have a social life, and return to work.
Risks
Risks
Risks from heart transplant include:
- Rejection of the donor heart.
- To check for rejection, surgeons will regularly test a sample (biopsy) of the heart tissue. They'll also do echocardiography, electrocardiography (ECG, EKG), or blood tests.
- If your body rejects the heart, you will receive other drugs (such as immunosuppressants or steroids) to suppress your immune system so that it does not reject the donor heart. These drugs may have serious side effects, including an increased risk of infections and cancer.
- Infection.
- Clogging of the arteries (atherosclerosis) that may develop in the donor heart. (This is usually a complication and can affect long-term survival.)
- Death.
References
References
Citations
- Lund H, et al. (2017). The Registry of the International Society for Heart and Lung Transplantation: Thirty-fourth Adult Heart Transplantation Report—2017. Focus theme: Allograft ischemic time. Journal of Heart and Lung Transplantation 36(10): 1037–1046. https://doi.org/10.1016/j.healun.2017.07.019. Accessed October 7, 2019.
Current as of: October 2, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Ignite Healthwise, LLC, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.
To learn more about Ignite Healthwise, LLC, visit webmdignite.com.
© 2024-2025 Ignite Healthwise, LLC.
Related Links
Organ Transplant
<cipublic-spinner variant="large"><span>Loading…</span></cipublic-spinner>